..."Researchers suggest, up to 90% of tattoo inks in the U.S. might be mislabeled. This isn’t just a case of a missing pigment or a minor discrepancy. These inks contained potentially concerning additives that weren’t listed on the packaging. More at The Conversation ➜
Public Posts Edmonds, WA Edmonds, WA (zoom)
"Reconnecting children and nature may be the last cause in America that transcends political, religious, racial, and professional barriers; it brings people to the same table who usually do not want to be in the same room. Again and again, I have seen conservatives and liberals, physicians and educators, conservationists and developers, and many others work together for this cause. No one wants to be in the last generation where it’s considered normal for a child to lay under a tree in the woods" More at The MIT Press Reader ➜
"Dietary supplements are a big business. The industry made almost US$39 billion in revenue in 2022, and has very little regulation and oversight...Supplements are regulated as food instead of drugs, even though they can interact with medications and may be laced with hidden drugs not included on the label....The FDA’s website states that “many dietary supplements contain ingredients that have strong biological effects which may conflict with a medicine you are taking or a medical condition you may have." More at The Conversation ➜
Over half of Stockton, California’s residents are diabetic or prediabetic. A prescribed meal program aims to change that. More at Reasons to be Cheerful ➜
No one told me it would be like this—
how growing older is another passage of discovery
and that aging is one grand transformation,
and if some things become torn apart
or even lost along the way,
many other means show up
to bring me closer
to the center of my heart.
No one ever told me
if whatever wonder waits ahead
is in another realm and outside of time.
But the amazement, I found,
is that the disconcerting things
within the here and now
that I stumble and trip my way through,
also lead me gracefully home.
And no one told me that I would ever see
an earth so strong and fragile,
or a world so sad and beautiful.
And I surely didn't know
I'd have all this life yet in me
or such fire inside my bones.
From Susan Frybort, (author of Open Passages) poetry collection "Look to the Clearing"
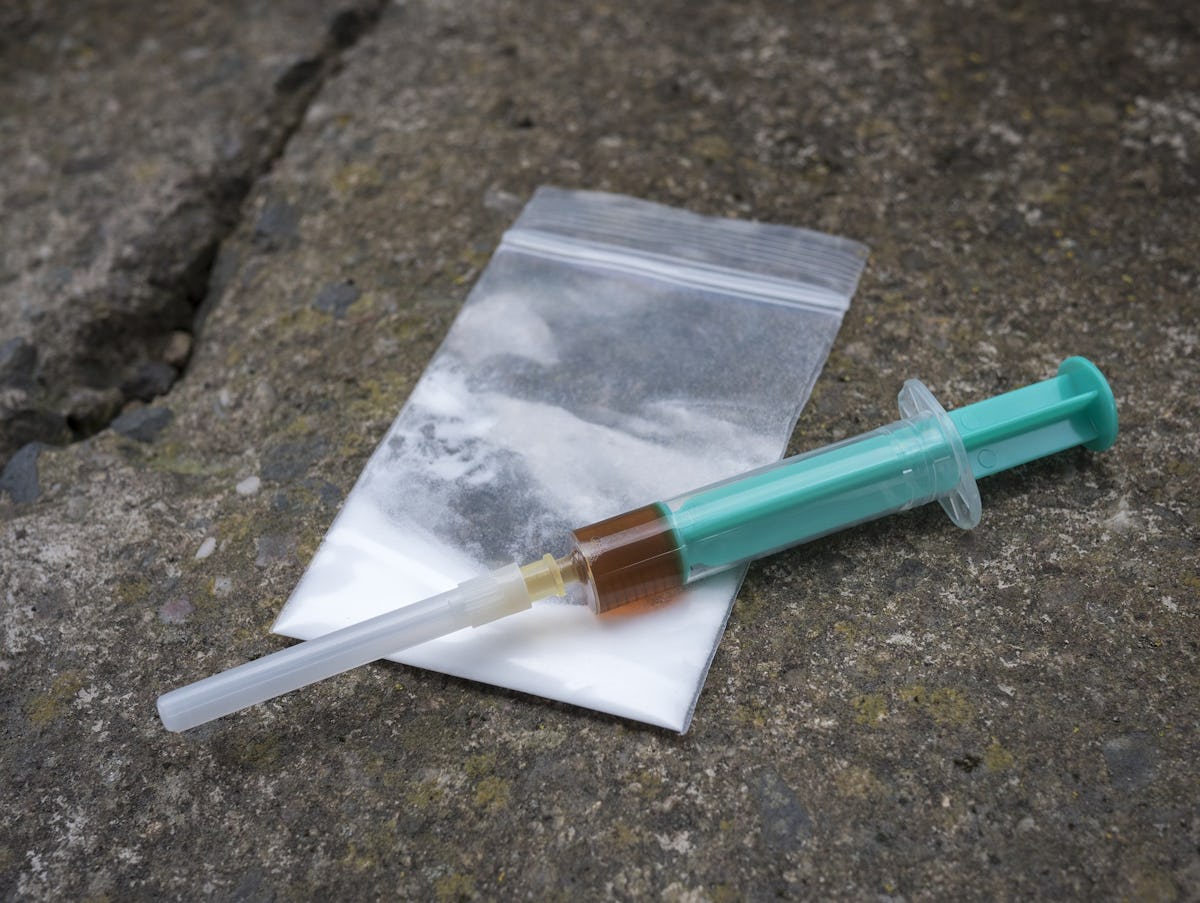
"It’s the big threat. A cheap, white powder — 50 times more powerful than heroin — which kills more than 70,000 people each year in the United States and countless others across the rest of the Western Hemisphere. EL PAÍS, in a long-term investigation that spanned two continents and included interviews with anti-drug czars in the U.S. and China, visited the clandestine laboratories in Sinaloa, where fentanyl is manufactured".......Read More at El Pais ➜ Also Read: How the United States got hooked on fentanyl
Many people are wired to seek and respond to rewards. Your brain interprets food as rewarding when you are hungry and water as rewarding when you are thirsty. But addictive substances like alcohol and drugs of abuse can overwhelm the natural reward pathways in your brain, resulting in intolerable cravings and reduced impulse control. More at The Conversation ➜
"This revolutionary prosthetic limb is giving amputees the chance to regain natural movement. Developed by bioengineers at Johns Hopkins University, the prosthetic limb connects directly to the wearer's peripheral nervous system. The limb is controlled by the wearer's own thoughts, allowing them to move the prosthesis with the same ease as a real limb. More at WIRED UK ➜
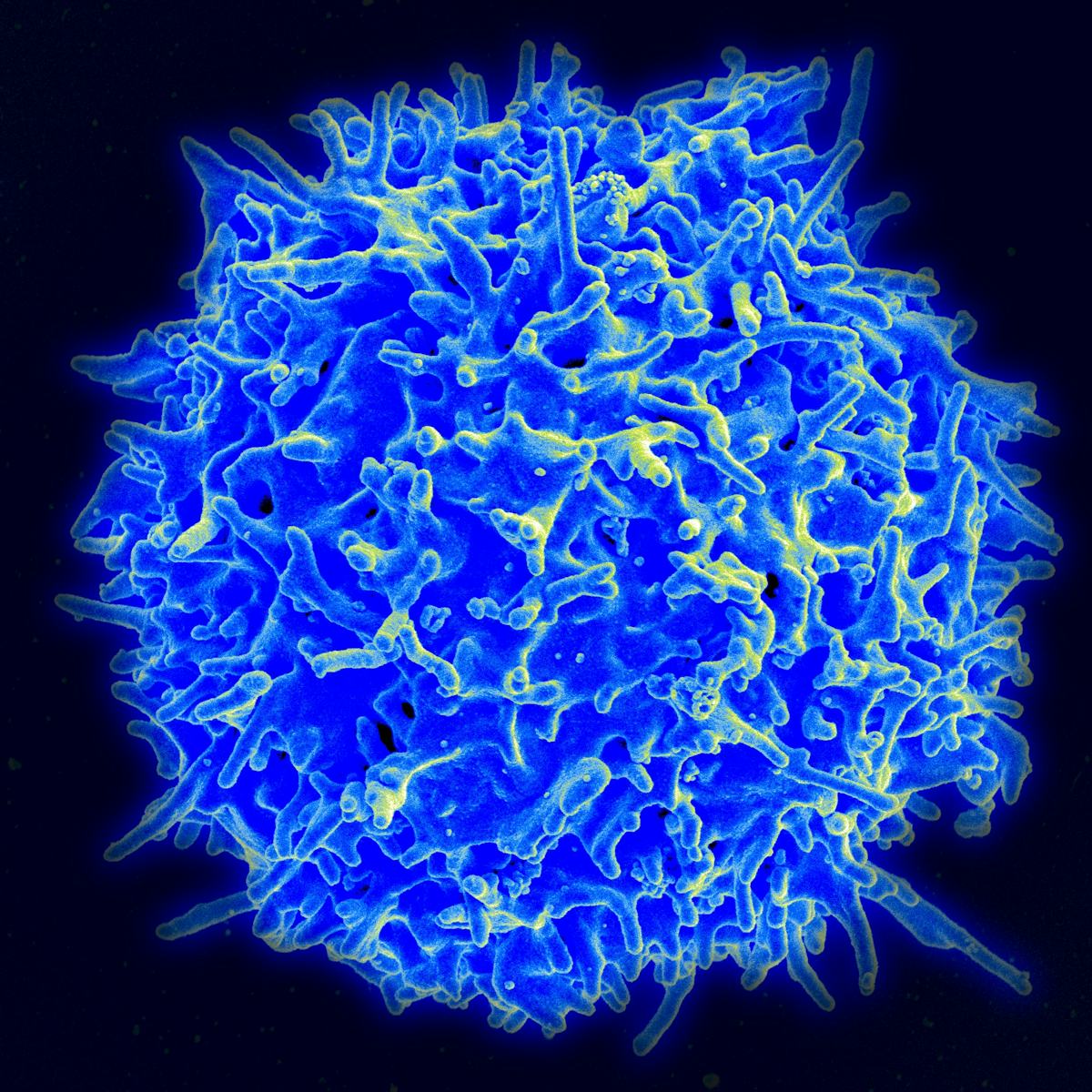
"Your immune system requires a delicate balance to operate properly. When it’s out of balance, your immune system itself can cause disease. Healthy immune systems don’t need to be “boosted.” ... immunologists know that too much of an immune reaction could result in allergies, autoimmune disorders or chronic inflammation. On the flip side, too little of an immune reaction could result in illness or infection" More at The Conversation ➜
Image credit: NIH NIAD (Scanning electron micrograph of a T cell)
I don't like it,
I never will,
when I see all
of the mentally ill.
The Residents, I know,
I know them still,
they are nice.
yet they are ill.
What kind of World
can this be,
when we live in
a mental society?
"First, the shrimp disappeared. In late 1980s, the catch became so poor that Diane Wilson, a fourth-generation shrimper, had to take a job running a fish house in Seadrift in Calhoun County, Texas, where she grew up and still lives. Then beached, diseased 300-pound dolphins started appearing, and dead pelicans kept floating to the shores of Lavaca Bay" More at Reasons to be Cheerful ➜
"A vaccine against tuberculosis, the world’s deadliest infectious disease, has never been closer to reality, with the potential to save millions of lives. But its development slowed after its corporate owner focused on more profitable vaccines" More at ProPublica ➜








.jpg?fit=crop&w=280&h=280&q=93)




.jpg?fit=crop&w=200&h=200&crop=faces)











 - Copy.jpg?fit=crop&w=280&h=280&q=93)














